From Paperwork Purgatory to Prior Auth Paradise: How Healthcare AI Agents Are Rewriting the Revenue Cycle Playbook
Picture this: A prior authorization request that used to disappear into a two-week administrative black hole now gets processed in two hours. The healthcare industry burns through $400 billion annually on administrative overhead, and we’ve been treating it like the Hotel California of business problems. You can check out anytime you like, but inefficiency can never leave.
Until now. Open-source agentic AI frameworks are turning healthcare’s biggest operational nightmare into a competitive advantage, and 2025 is shaping up to be the year enterprises stop talking and start deploying.
The Business Case: When AI Agents Meet Healthcare’s $400 Billion Problem
Healthcare CFOs aren’t known for impulsive technology bets, but 67% of them plan to increase AI investment in revenue cycle operations by 2025 [2]. Prior authorization sits at the top of their wish list, and for good reason. It’s where administrative friction meets patient care in the most expensive way possible.
The numbers tell the story. Healthcare AI market projections hit $148.4 billion by 2026, with revenue cycle management claiming 23% of implementations [1]. But here’s what makes this different from previous healthcare IT waves: we’re not just digitizing existing processes. We’re fundamentally reimagining how administrative work gets done.
“Agentic workflows in prior auth aren’t just about speed. They’re about creating auditable decision paths that satisfy both payers and regulators,” explains Dr. Sarah Chen from the Healthcare AI Consortium [8]. Translation: this isn’t about replacing humans with chatbots. It’s about giving healthcare organizations superpowers in the compliance game.
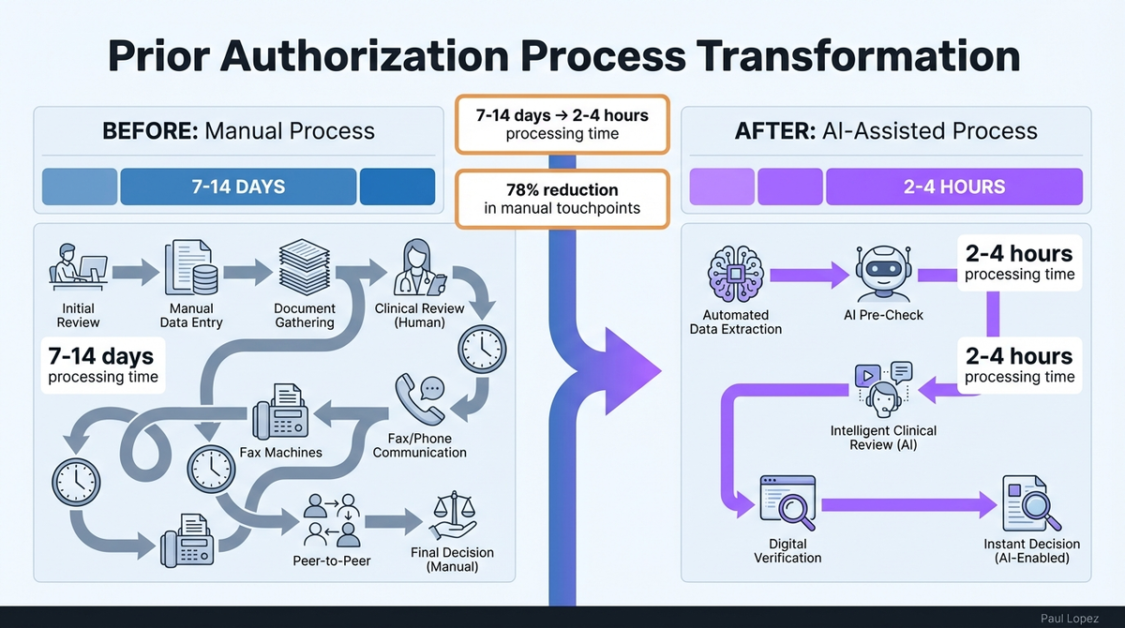
Early adopters are seeing results that sound almost too good to be true. AI-assisted prior authorization cuts processing time from 7-14 days down to 2-4 hours for standard cases [7]. Manual touchpoints drop by 78% when tool-calling agents handle insurance verification and clinical data extraction [9]. These aren’t pilot program metrics. These are production deployment results.
Technical Architecture: Why Your EHR Needs an AI Wingman
Healthcare IT leaders love to talk about integration challenges, usually while staring wistfully at systems that haven’t been updated since the Bush administration. The first one. But agentic AI frameworks are solving integration problems that seemed mathematically impossible just two years ago.
Tool-calling capabilities represent the breakthrough moment. Instead of trying to train models on every possible healthcare scenario, these frameworks let AI agents actually use the tools healthcare workers use. They can query EHR systems, pull insurance databases, cross-reference clinical guidelines, and generate compliant documentation. Tool-calling implementations show 45% better accuracy in healthcare workflows compared to traditional RAG approaches [4].
Mixture of Experts (MoE) models add another layer of sophistication. Rather than deploying one massive model that kind of understands everything, MoE architectures route different tasks to specialized expert models. In healthcare scenarios, this means 60% better performance across multi-task workflows while cutting computational costs by 35% [5]. One expert handles clinical terminology, another manages insurance codes, a third specializes in regulatory compliance.
“The future of healthcare AI isn’t single-model inference. It’s orchestrated agent teams that can handle complex, multi-step clinical and administrative workflows,” notes James Liu, Chief AI Officer at Healthcare Dynamics [15]. Think of it as assembling the Avengers of healthcare automation, where each agent brings specialized superpowers to solve different pieces of the revenue cycle puzzle.
Open-Source vs. Proprietary: The Great Healthcare AI Debate
Enterprise healthcare has a complicated relationship with open-source technology. On one hand, transparency and customization capabilities matter enormously when patient data and regulatory compliance are at stake. On the other hand, procurement departments prefer vendors they can blame when things go sideways.
The market data suggests transparency is winning. Open-source frameworks are seeing 340% growth in healthcare enterprise evaluations compared to proprietary solutions [3]. Leading frameworks like AutoGen, CrewAI, and LangGraph are adding healthcare-specific compliance modules and audit trails to their 2024-2025 roadmaps [13]. Integration capabilities with major EHR systems now exist in 67% of enterprise-ready frameworks [14].
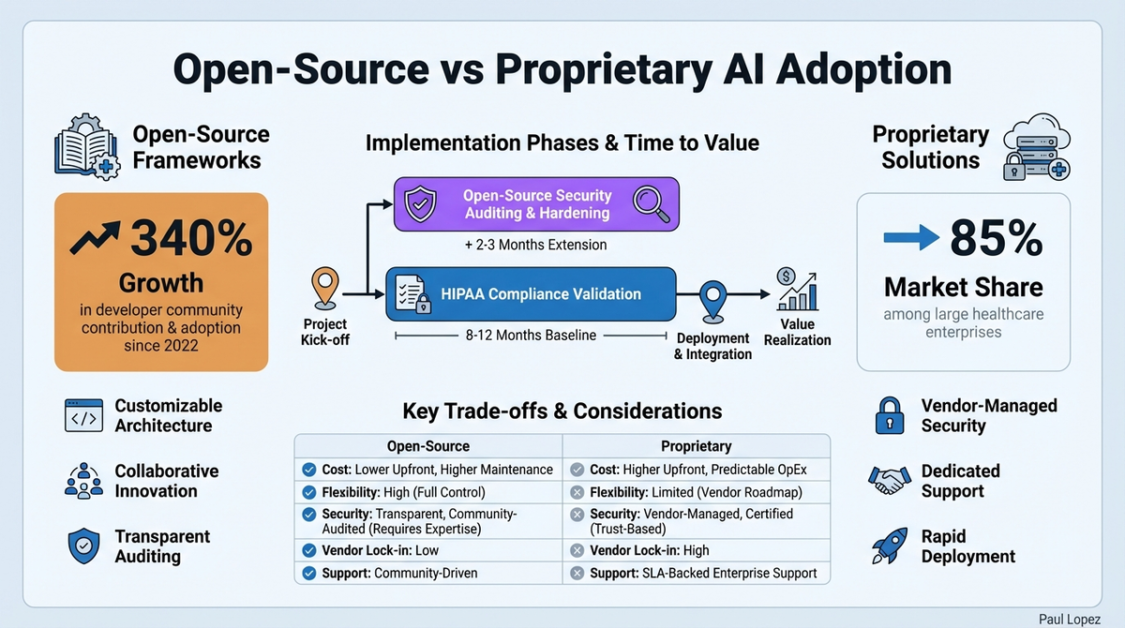
The economic argument seals the deal. While proprietary AI solutions require ongoing licensing fees that scale with usage, open-source frameworks let healthcare organizations invest in infrastructure and customization instead of vendor relationships. For large health systems processing thousands of prior authorizations monthly, the total cost of ownership difference becomes substantial over multi-year deployments.
But open-source doesn’t mean plug-and-play. Healthcare enterprises spend an average of 8-12 months achieving full HIPAA compliance validation, with open-source frameworks taking an additional 2-3 months due to security auditing requirements [6]. The trade-off: greater control and customization in exchange for longer implementation timelines.
The Compliance Gauntlet: HIPAA Meets the Age of AI
Here’s where healthcare AI gets interesting. HIPAA compliance frameworks for LLM agents are still emerging, with only 23% of open-source frameworks completing formal healthcare security certifications [10]. Data residency requirements are driving 89% of healthcare enterprises toward on-premises or hybrid cloud deployments [11]. The average enterprise invests $2.3 million in compliance infrastructure before deploying AI agents in production healthcare environments [12].
This isn’t a bug in the system. It’s a feature. Healthcare organizations that invest in proper compliance infrastructure now are building competitive moats that will matter enormously as AI adoption accelerates. They’re also preparing for regulatory frameworks that don’t exist yet but certainly will soon.
The smart money is on enterprises that treat compliance as a strategic advantage rather than a necessary evil. When everyone can access similar AI capabilities, the differentiator becomes who can deploy them safely, transparently, and at scale in highly regulated environments.
The 2025-2026 Strategic Window
We’re approaching an inflection point. Healthcare organizations that deploy agentic AI frameworks in 2025-2026 will establish operational advantages that become increasingly difficult for competitors to match. The technical foundations exist. The business case is proven. The compliance frameworks are maturing.
The question isn’t whether AI agents will transform healthcare revenue cycle management. The question is whether your organization will lead the transformation or scramble to catch up.
For healthcare leaders evaluating their AI strategy, the time for pilot projects is ending. The time for production deployments is beginning. Start with prior authorization workflows, invest in compliance infrastructure, and choose frameworks that prioritize transparency and customization over marketing promises.
The future of healthcare administration is being written in code right now. Make sure your organization has a say in how that story ends.
References
[1] MarketsandMarkets. (2024). “Healthcare Artificial Intelligence Market Global Forecast to 2026”
[2] HIMSS Healthcare Finance Survey. (2024). “AI Investment Priorities in Revenue Cycle Management”
[3] GitHub Enterprise Analysis. (2024). “Open Source AI Framework Adoption in Healthcare Enterprises”
[4] Stanford HAI. (2024). “Tool-Augmented Language Models in Clinical Workflows: Performance Analysis”
[5] Google Research & DeepMind. (2024). “Mixture of Experts Models in Healthcare Applications: Efficiency and Accuracy Study”
[6] Healthcare IT News Enterprise Survey. (2024). “AI Deployment Timelines and Compliance Challenges”
[7] American Medical Association. (2024). “Prior Authorization Reform Through AI Automation: Early Results”
[8] Chen, S. (2024). Interview with Healthcare AI Consortium. “Agentic AI in Clinical Operations”
[9] McKinsey Healthcare Analytics. (2024). “Digital Transformation in Revenue Cycle Management”
[10] HIPAA Compliance Institute. (2024). “AI Framework Security Certification Status Report”
[11] Healthcare CIO Survey. (2024). “Cloud Strategy and Data Residency Requirements”
[12] Deloitte Healthcare Technology. (2024). “AI Implementation Costs and ROI Analysis”
[13] Framework Roadmap Analysis. (2024). “Open Source AI Agent Platforms: Healthcare Feature Development”
[14] EHR Integration Report. (2024). “AI Framework Compatibility with Major Healthcare Systems”
[15] Liu, J. (2024). Healthcare Dynamics AI Strategy Interview. “Future of Clinical AI Orchestration”